A Clinical Comparison of Modern Structural Adipose FillersAn Evidence-Informed Overview for Aesthetic and Regenerative PractitionersAdvances in soft-tissue augmentation have expanded far beyond traditional hyaluronic-acid fillers. Modern regenerative aesthetics now includes biologically derived structural fillers such as AlloClae—a donor-derived adipose matrix designed to mimic aspects of fat grafting without the requirement for liposuction or surgery.At the …
A Clinical Comparison of Modern Structural Adipose Fillers
An Evidence-Informed Overview for Aesthetic and Regenerative Practitioners
Advances in soft-tissue augmentation have expanded far beyond traditional hyaluronic-acid fillers. Modern regenerative aesthetics now includes biologically derived structural fillers such as AlloClae—a donor-derived adipose matrix designed to mimic aspects of fat grafting without the requirement for liposuction or surgery.
At the same time, autologous fat grafting (AFT) remains the gold standard for patients with adequate donor fat, thanks to its unmatched cellular/regenerative properties, longevity, and natural integration.
This article examines both modalities—what AlloClae is, its advantages and limitations, and why autologous fat remains superior when available, allowing clinicians to select the best option for each patient.
What Is AlloClae?
AlloClae is an acellular human adipose-derived structural filler. Donor fat is processed to remove all living cells (including immunogenic adipocytes), while preserving:
- the extracellular matrix (ECM)
- structural proteins (collagen, elastin)
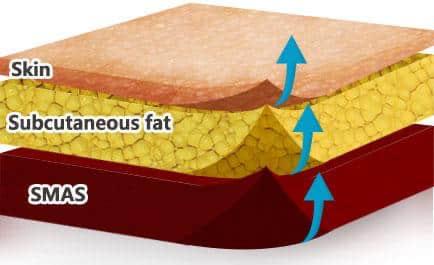
- the native “honeycomb” scaffold of adipose tissue
- embedded growth factors
This results in a biocompatible, sterile, ready-to-inject adipose matrix designed to provide structural volume without the need for liposuction, fat harvesting, or surgical grafting.
Its goal is to bridge the gap between fat transfer and synthetic fillers by offering:
- biological softness
- tissue integration potential
- convenience of an injectable filler
- suitability for patients with minimal donor fat
***Read More: Optimal Anatomical Planes for Dermal Filler Injection
How AlloClae Works Biologically
Because the ECM architecture is preserved, AlloClae acts as a scaffold that allows:
- host-cell infiltration
- neovascularization
- collagen remodeling
- gradual incorporation into soft tissue
It does not contain living adipocytes or stem cells, so volume retention depends on host repopulation and ECM remodeling rather than survival of grafted fat.
Clinical Advantages of AlloClae
✔ No Surgery or Fat Harvesting
Ideal for:
- lean patients lacking donor fat
- patients unwilling or unable to undergo liposuction
- quicker, low-morbidity procedures
✔ Minimally Invasive With Rapid Recovery
Delivered via needle/cannula under local anesthesia with minimal downtime.
✔ Immediate Volume + Natural Biological Texture
The preserved ECM provides:
- soft, natural feel
- structural support
- potential long-term textural improvements
✔ Versatility
Suitable for:
- hip dips
- buttock contour refinement
- thigh or hip shaping
- breast symmetry correction
- scar/indentation filling
- moderate volume replacement after weight loss
Limitations and Clinical Considerations
⚠ Partial Resorption (Not Permanent)
Most patients experience some loss of volume over 12–24 months.
⚠ Limited Long-Term Data
As a relatively new product, robust peer-reviewed evidence is still evolving.
⚠ Cost
More expensive than HA fillers; multiple syringes may be required for body areas.
⚠ Volume Limits
Not ideal for large-volume augmentation (e.g., full BBL); better for moderate contouring.
⚠ Donor-Derived Tissue
Although processed to reduce immunogenicity, long-term behavior is still under investigation.
When AlloClae Is Especially Useful
AlloClae is an excellent choice for:
- lean patients without harvestable fat
- individuals who want moderate corrections, not dramatic augmentation
- patients who want no downtime
- refining hip dips, contour irregularities, or small breast asymmetries
- those seeking a more natural-feeling alternative to synthetic fillers
It fills an important niche: a regenerative scaffold for patients who cannot undergo traditional fat grafting.
Why Autologous Fat Grafting Remains the Gold Standard
If a patient does have donor fat, autologous fat grafting is biologically and clinically superior.
Fat Contains Living Adipocytes + Regenerative ADSCs
Autologous fat includes:
- adipose-derived stem cells (ADSCs)
- pericytes
- pre-adipocytes
- viable adipocytes
These cells promote:
- angiogenesis
- tissue regeneration
- long-term graft survival
- reduced fibrosis
- improved skin quality
No off-the-shelf filler—including AlloClae—can replicate this living regenerative biology.
Superior Longevity (Often Permanent)
With modern techniques (microfat, low-shear harvest, micro-parcel injection), fat survival rates are typically 50–70%, with results lasting years or even permanently.
- Zero Immunogenicity
Because the tissue is autologous:
- no allergic reactions
- no foreign-body response
- no risk of granuloma from donor proteins or cross-linkers
***Read More : RF Microneedling
Most Natural Look and Dynamic Behavior
Fat integrates physiologically:
- soft, natural contour
- changes with patient weight
- ages with the person
- best for high-volume areas
Most Cost-Effective for Larger Volumes
For >50–100 mL:
- AlloClae becomes expensive
- HA fillers are impractical
- Fat grafting becomes the most efficient, long-term solution
Thus, for buttocks, hips, breasts, thighs, or overall body shaping, autologous fat is unmatched.
Clinical Decision-Making: When to Use What
Treatment Best For Longevity Pros Cons
Autologous Fat Patients with donor fat, large areas, long-term results Very long term / permanent ADSCs, natural, high volume Requires liposuction
AlloClae Lean patients, moderate volume, low downtime 12–24+ months Biological scaffold, soft feel Costly, limited long-term data
Synthetic Fillers (HA, etc.) Precision work, reversible treatments 6–18 months Shape control, fully reversible Not suitable for large volumes
Conclusion
AlloClae represents an exciting evolution in adipose-based regenerative fillers, offering a biologically derived, minimally invasive option for patients who lack donor fat or prefer to avoid surgery.
However—in patients with sufficient fat reserves, autologous fat grafting remains biologically superior, thanks to its stem-cell content, natural integration, and long-term or permanent outcomes.
Together, these modalities give clinicians the flexibility to design highly personalized treatment plans based on patient anatomy, goals, and tolerance for downtime.
Each has a place, but fat is still the gold standard, and AlloClae is an excellent second-best option for appropriately selected patients.
References
AlloClae / Structural Adipose Matrix
- SoCal Plastic Surgeons — AlloClae Expert Guide.
- R. Rahban MD — AlloClae Overview.
- PFrankMD — AlloClae Injectables.
- Glenn Lyle MD — Natural Volume Restoration with AlloClae.
- Simple Aesthetics — AlloClae Overview.
- Zuri Plastic Surgery — AlloClae for Lean Patients.
- Austin Plastic Surgeon — “How AlloClae Is Transforming Body Contouring for 2025.”
- Beautyfix MedSpa — AlloClae Benefits & Considerations.
Autologous Fat, ADSCs & Graft Survival
- Coleman SR. Structural Fat Grafting. Plast Reconstr Surg.
- Eto H et al. Fat Graft Survival and ADSCs. Plast Reconstr Surg.
- Kaufman MR et al. Comparison of Fat Grafting and Fillers. Aesthetic Surg J.
- Zuk PA et al. ADSCs: Multilineage Cells From Adipose Tissue. Tissue Eng.
- Review on ADSCs in Regeneration. Diabetes Care.